What is an IBS flare-up?
An IBS flare-up is a temporary worsening of gut symptoms – cramping, bloating, and changes in bowel habits – that can last anywhere from a few hours to a few days, and almost always passes.
The terms ‘IBS flare-up and ‘IBS attack’ are often used interchangeably. Both describe a sudden worsening of symptoms – the difference is mainly intensity, with an attack typically referring to something more severe or prolonged. There is no clinical distinction between them.
Flare-ups can be triggered by stress, food, hormonal changes, or a gut infection – and sometimes they strike with no clear cause at all. Understanding what's driving yours, and what you can do when one hits, makes them much easier to manage.
What triggers an IBS flare-up?
Because IBS is a gut-brain disorder, triggers don't cause structural damage to the gut – they activate a nervous system that's already oversensitive. This is also why flare-ups can sometimes occur with no clear trigger at all.
Common triggers include:
Stress and psychological factors
Both short-term and chronic stress can heighten gut sensitivity and alter how the intestines move. Anxiety and depression also intensify gut-brain signaling – which is why emotional and digestive symptoms so often arrive together.1
High FODMAP foods
Fermentable carbohydrates – including fructans (garlic, onion, wheat), lactose (dairy), fructose (apples, honey, mango), and polyols (mushrooms, cauliflower, stone fruits) – are poorly absorbed in the small intestine and ferment in the gut, producing gas and triggering symptoms.
Hormonal changes
Many people with IBS notice symptoms worsen at certain points in their menstrual cycle, reflecting how sex hormones interact with gut-brain signaling.
Gut infections
Gastroenteritis or food poisoning can trigger a period of heightened gut sensitivity – sometimes developing into post-infectious IBS, where symptoms persist long after the infection has cleared.2
Caffeine and alcohol
Both can stimulate the intestines and lower the threshold for symptoms, particularly diarrhea and urgency.
Why IBS is a gut-brain disorder
IBS is not just a digestive condition – it is a gut-brain disorder, meaning the problem lies in how the gut and brain communicate rather than in any structural damage to the digestive tract.3
In people with IBS, this communication becomes dysregulated, making the gut oversensitive. Normal digestive activity – gas, movement, pressure – gets processed as pain or discomfort that most people would never notice. During a flare-up, this oversensitivity is at its peak, which is why symptoms can feel so intense and unpredictable even when nothing has visibly changed.
"Symptoms are very real and they are driven by what happens between the gut and the brain and the brain to the gut along what's called the brain-gut axis." – Dr. Megan Riehl, GI Psychologist, Clinical Director of the GI Behavioral Health Program at the University of Michigan
IBS is the most common gut-brain disorder, but it isn't the only one. Functional dyspepsia, reflux hypersensitivity, and other conditions share the same underlying mechanism – an oversensitive gut-brain connection that can drive flare-ups in similar ways.
This short video explains what a gut-brain disorder is, how the gut-brain axis works, and why IBS is considered a gut-brain condition.
Even in conditions like IBD and GERD, where there is a structural or inflammatory component, research suggests that gut-brain dysregulation often plays a role in ongoing symptoms – particularly when symptoms persist despite treatment.
This is why treatment approaches that calm the nervous system, rather than just managing symptoms in the moment, tend to produce the most lasting relief.
How long does an IBS flare-up last?
Most IBS flare-ups peak within 2–4 days and then ease on their own, though some can linger for a week or more depending on the trigger and how quickly you're able to address it.
Duration varies widely from person to person. Some people experience a sharp flare that resolves within hours; others find symptoms come and go in waves over several weeks.
A number of factors influence how long a flare-up lasts – including what triggered it, stress levels at the time, and whether you're able to make adjustments to your diet or routine while symptoms are active.
The good news is that flare-up duration tends to shorten with better management. People who understand their triggers, have strategies in place, and are actively working on the gut-brain connection through approaches like gut-brain therapy often find their flare-ups become less frequent and easier to recover from over time.
What are the symptoms of an IBS flare-up?
The most common symptoms of an IBS flare-up are abdominal cramping, bloating, and changes in bowel habits – though the experience varies widely between people and between episodes.
Abdominal pain and cramping
Often the most disruptive symptom, ranging from a dull ache to sharp spasms that come and go in waves.
Bloating and abdominal swelling
The abdomen can feel visibly distended and uncomfortable, often worsening as the day goes on.
Changes in bowel habits
This may mean diarrhea, constipation, or alternating between both – sometimes within the same flare-up.
Gas and urgency
Excessive gas and a sudden urgent need to use the bathroom are common, and can make flare-ups particularly hard to manage in daily life.
A sense of incomplete emptying
Many people feel they haven't fully emptied their bowels after going to the bathroom, which can add to discomfort and frustration.
Some people also notice symptoms beyond the gut during a flare-up – including fatigue, headaches, heightened anxiety, and difficulty concentrating. This reflects how closely the gut and brain are connected: when one is under stress, the other often feels it too.

Brain-gut therapy, tailored to you
Fix the miscommunication between your back and brain
Overcome life's challenges
Take control of hot flashes and night sweats
Quit smoking in 3 weeks
What to eat during an IBS flare-up
The best foods to eat during an IBS flare-up are low FODMAP – gentle on the gut, easy to digest, and unlikely to ferment and worsen symptoms when your gut-brain system is already on high alert.
FODMAPs are fermentable carbohydrates that are poorly absorbed in the small intestine. In people with IBS and other gut-brain disorders, they can trigger bloating, cramping, and changes in bowel habits – particularly during a flare when gut sensitivity is at its peak.4 Temporarily reducing high FODMAP foods while IBS symptoms are active can help calm things down faster.
Foods to avoid during an IBS flare-up
High FODMAP foods that commonly worsen IBS symptoms include onion, garlic, wheat, rye, apples, mangoes, watermelon, honey, cow's milk, yogurt, ice cream, chickpeas, lentils, mushrooms, and cauliflower.
Foods that are easier to tolerate
Gentler, low FODMAP options include white rice, basmati rice, gluten-free oats, chicken, fish, cooked carrots, potatoes, kale, and small portions of nuts like pecans and pine nuts.
"Because at the end of the day, food is celebratory. It's cultural. It brings joy. We don't want patients to feel like they have to stick with a really strict diet." – Morgan Binder, Physician's Assistant and Registered Dietitian, Arizona Digestive Health
A low FODMAP diet works best as a short-term tool during an IBS flare-up, not a permanent way of eating. The goal is to identify your personal triggers over time – not to restrict forever.
How to calm an IBS flare-up
The most effective way to manage an IBS flare-up is to combine short-term symptom relief with approaches that address the gut-brain connection directly – calming the nervous system, not just the gut.
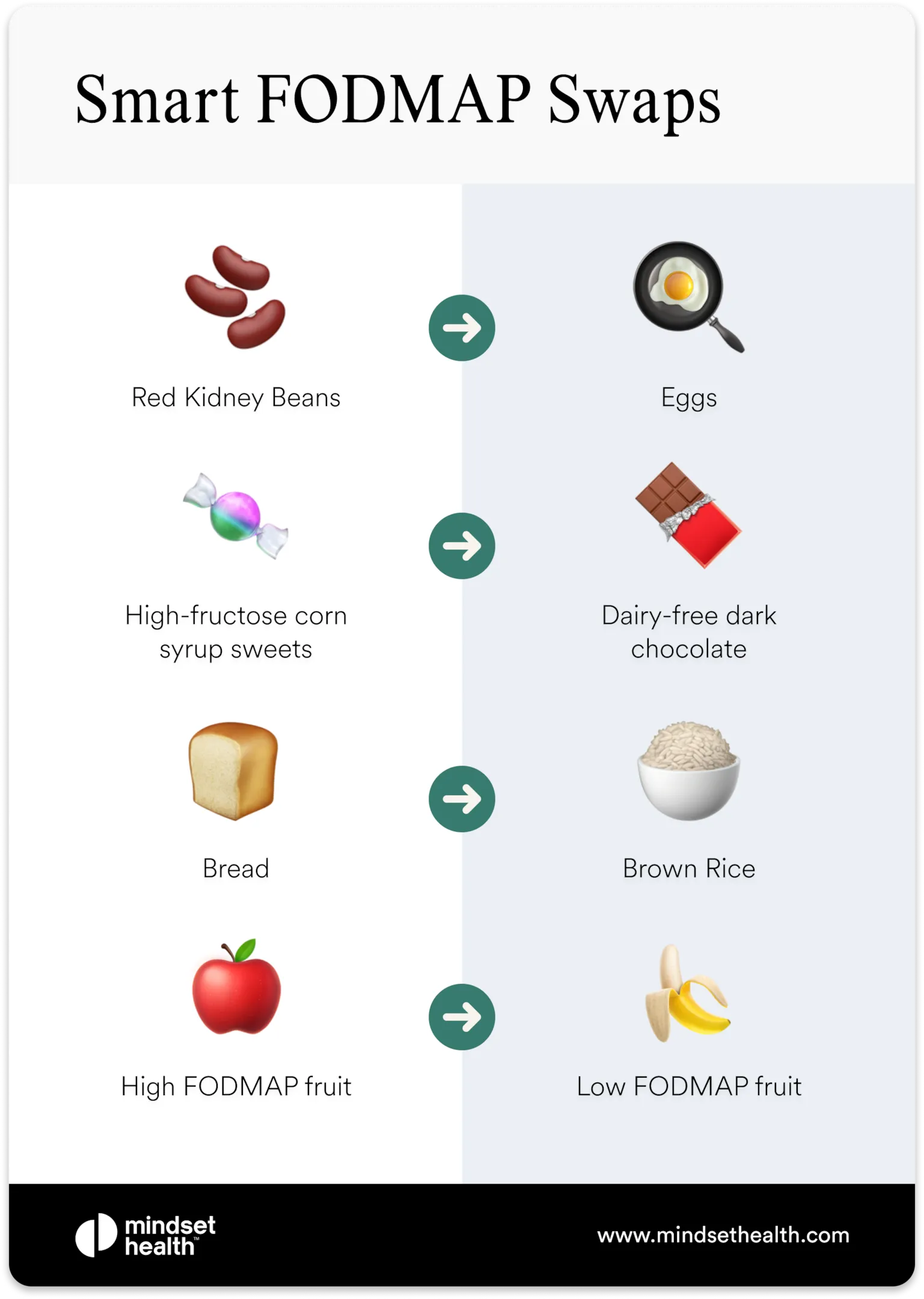
Switch to low FODMAP foods temporarily
Switching to low FODMAP foods while symptoms are active gives the gut less to react to. This doesn't need to be permanent – just a short-term reset while the flare settles.
Apply gentle heat
A warm heat pack or hot water bottle placed over the abdomen for 15–20 minutes can relax the muscles of the gut and ease cramping. It's simple, drug-free, and many people find it offers quick relief.
Reduce caffeine and alcohol
Both stimulate the intestines and can worsen diarrhea and urgency during a flare. Cutting them out temporarily – including coffee, tea, energy drinks, and alcohol – can make a noticeable difference.
Move gently
Light exercise like walking or gentle yoga helps regulate gut motility and reduces the stress hormones that fuel flare-ups. It doesn't need to be intense – even 15–20 minutes can help.
Try gut-brain therapy
Because IBS is a gut-brain disorder, approaches that calm the nervous system can reduce both the frequency and intensity of flare-ups over time. Gut-directed hypnotherapy works by retraining the communication between the gut and brain, reducing the oversensitivity that makes flare-ups so disruptive.
Manage stress actively
Stress is one of the most consistent IBS flare triggers. Mindfulness, breathing exercises, and relaxation techniques all help regulate the gut-brain response – and can shorten a flare when used during one.
How to manage an IBS flare-up with gut-brain therapy
Because IBS is a gut-brain disorder, one of the most effective ways to reduce flare-up frequency and intensity is to address the gut-brain connection directly – not just manage symptoms in the moment.
The same applies to other gut-brain disorders like functional dyspepsia and reflux hypersensitivity, where the underlying mechanism is the same: an oversensitive nervous system amplifying normal digestive signals.
Nerva is a 6-week gut-brain therapy program that uses gut-directed hypnotherapy to retrain communication between the gut and brain, reducing the oversensitivity that drives flare-ups. Completed at home in 15–20 minutes a day, it is guideline-recommended for gut-brain disorders by major gastroenterology bodies, including the American College of Gastroenterology, NICE, and the Rome Foundation.5
Around 80% of Nerva users report improved symptom management regardless of their triggers – whether food, stress, or hormonal changes.
In a randomized controlled trial published in the American Journal of Gastroenterology, 81% of Nerva participants achieved a clinically significant improvement in IBS symptoms, and 71% had a clinically significant reduction in abdominal pain.6
"Gut-directed hypnotherapy also shows similar rates of symptom improvement to the low FODMAP diet, which is currently considered as the first-line therapy for IBS." – Ellie Anderson, Accredited Practicing Dietitian, Mine and Gut Clinic, Melbourne; PhD Candidate at Monash University
Medical treatments for IBS flare-ups
When lifestyle and gut-brain approaches aren't enough, a doctor may recommend medication to help manage IBS symptoms. Common options include:
Antispasmodics
These relax the muscles of the colon to ease cramping and spasms during a flare-up. Common examples include hyoscine and dicyclomine.
Antidiarrheals
Medications like loperamide can help control severe diarrhea during a flare. These should be used under medical guidance.
Low-dose antidepressants
Low-dose tricyclic antidepressants or SSRIs are sometimes prescribed to help regulate the gut-brain connection and manage abdominal pain. These should always be prescribed and monitored by a doctor.
When to see a doctor about IBS flare-ups
Most IBS flare-ups can be managed at home, but some symptoms warrant prompt medical attention – particularly if they are new, worsening, or don't fit your usual pattern.
See a doctor as soon as possible if you experience any of the following:
Blood in your stool
Any rectal bleeding or dark, tar-like stools should always be investigated – this is not a typical IBS symptom.
Unexplained weight loss
Losing weight without trying, particularly alongside digestive symptoms, needs medical assessment.
Symptoms that wake you at night
IBS symptoms typically don't disturb sleep. If pain or urgency is waking you, something else may be going on.
Persistent or worsening pain
Pain that doesn't ease between flare-ups, or that is steadily getting worse over time, needs evaluation.
Fever, nausea, or vomiting
These are not typical IBS symptoms and may indicate infection or another condition requiring treatment.
New symptoms after age 50
Any significant change in bowel habits or new digestive symptoms in people over 50 should be discussed with a doctor promptly.
IBS is a diagnosis of exclusion – meaning other conditions need to be ruled out first. If you haven't yet received a formal diagnosis, or if your symptoms have changed significantly, a consultation with a gastroenterologist is always worthwhile.
Frequently asked questions
How do I know if my IBS is flaring up?
A flare-up is when your usual IBS symptoms become more intense or frequent than your normal baseline – typically stronger cramping, noticeable bloating, and a clear shift in bowel habits. If symptoms feel worse than your day-to-day normal and are disrupting your routine, it's likely a flare.
Why do I keep getting IBS flare-ups even when I eat well?
Food is only one trigger for IBS flare-ups. Because IBS is a gut-brain disorder, stress, hormonal changes, and anxiety can all activate an oversensitive nervous system and cause symptoms – regardless of what you've eaten.
Can stress cause a physical IBS flare-up?
Yes. Stress directly affects gut function in people with IBS by altering gut motility and lowering the pain threshold. This is because IBS involves dysregulated communication between the gut and brain, meaning emotional and physical symptoms are genuinely connected.
How long does an IBS flare-up usually last?
Most IBS flare-ups peak within 2–4 days and ease on their own. Some can last a week or more, depending on the trigger and how quickly you're able to manage it.
What is the fastest way to calm an IBS flare-up?
Switching to low FODMAP foods, applying gentle heat to the abdomen, and reducing caffeine can all help ease symptoms quickly. Addressing the stress response at the same time – through breathing exercises or gut-brain therapy – tends to shorten a flare faster than diet changes alone.
Can gut-brain therapy reduce IBS flare-ups?
Yes. Programs like Nerva target the underlying nervous system sensitivity that drives flare-ups, rather than just managing symptoms in the moment. In a randomized controlled trial, 81% of Nerva participants achieved clinically significant improvement in IBS symptoms.